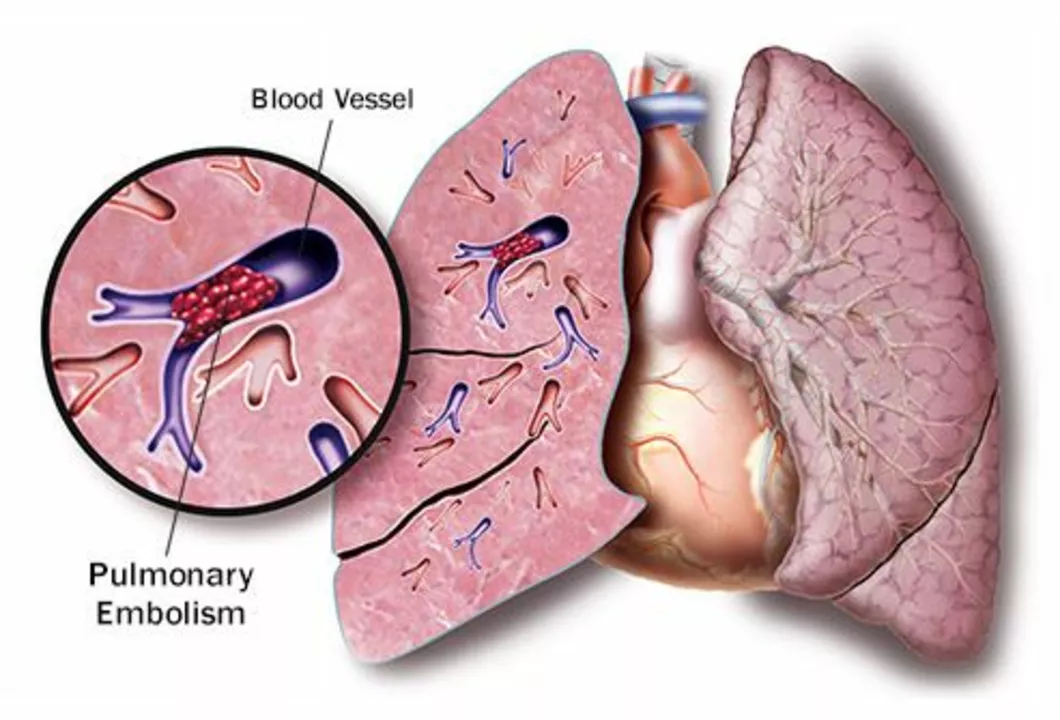
Pulmonary Embolism – What It Is, How to Spot It, and What to Do
Imagine a blood clot suddenly blocking an artery in your lung. That’s a pulmonary embolism (PE), and it can turn a normal day into a medical emergency within minutes. The good news? Knowing the warning signs and acting fast can save lives.
Key Symptoms You Shouldn't Ignore
Most people think PE only causes chest pain, but it often shows up as a mix of symptoms:
- Sudden shortness of breath: Even if you were just sitting, you might feel like you can’t get enough air.
- Sharp or stabbing chest pain: The pain usually gets worse when you breathe deep or cough.
- Rapid heartbeat: Your pulse may race without any obvious reason.
- Cough with blood‑tinged sputum: This isn’t common, but it can happen.
- Dizziness or fainting: A big clot can lower oxygen levels enough to make you feel light‑headed.
If any of these appear out of the blue—especially after a long flight, surgery, or period of immobility—call emergency services right away.
Major Risk Factors and Prevention Tips
Knowing what puts you at risk helps you take steps before a clot forms. The biggest culprits are:
- Prolonged inactivity: Sitting for hours on a plane or during recovery from surgery lets blood pool in your legs.
- Recent surgery or trauma: The body’s clotting system kicks into high gear after an operation.
- Medical conditions: Cancer, heart failure, and inherited clotting disorders raise the odds.
- Hormonal factors: Birth control pills, hormone therapy, or pregnancy increase clot risk.
- Obesity and smoking: Both strain circulation and promote clot formation.
Simple habits can lower those risks: move around every hour on long trips, stay hydrated, wear compression stockings if your doctor recommends them, and keep a healthy weight. If you have a known clotting disorder, follow your doctor’s anticoagulant plan exactly.
When a PE is suspected, doctors usually run a CT scan or a ventilation‑perfusion (V/Q) lung scan to confirm the blockage. Blood tests for D‑dimer can also hint at a clot.
Treatment focuses on stopping the clot from growing and preventing new ones. Anticoagulants like heparin or newer oral agents are first‑line. In severe cases, doctors may use clot‑busting drugs (thrombolytics) or even surgery to remove the blockage.
Recovery time varies. Many people can return to normal activities within weeks if they stick to their medication schedule and avoid long periods of immobility.
Bottom line: Pulmonary embolism is scary, but it’s also treatable when caught early. Keep an eye on the symptoms, know your personal risk factors, and don’t hesitate to seek help if something feels off. Your lungs deserve swift action—don’t wait.
The Psychological Impact of Pulmonary Embolism: Coping with Anxiety and Fear
As a pulmonary embolism survivor, I can't stress enough the psychological impact this condition has had on my life. The constant anxiety and fear of another clot forming have become an overwhelming part of my daily routine. In my journey to cope, I've found that talking to a therapist, joining support groups, and practicing mindfulness have greatly helped in easing my worries. Additionally, educating myself about my condition and knowing the warning signs has given me a sense of control. Remember, you're not alone in this battle, and seeking help is crucial for your mental well-being.
read more